AUTHORS
Heather Adams PhD, LAT, ATC, CHSE1; John Kiesel PT, DPT, PhD, CHSE1; Brandi Andreae OTD, MS, OTR, CHSE1; Kailee Burdick DNP, RN, CNE, CHSE2; Chelsea Elwood DMS, MS, PA-C 1; JoEllen Henson DHSc, MSW, LSW, MSEd3; Laura Livingston BSN, RN, CHSE2; Nicole Mix PT, DPT, PhD, CHSE1
1Department of Applied Medicine and Rehabilitation, Indiana State University, Terre Haute, IN
2Rural Health Innovation Collaborative Simulation Center, Terre Haute, IN
3Department of Social Work, Indiana State University, Terre Haute, IN
Corresponding Author: Heather Adams, heather.adams@indstate.edu
Conflict of interest statement: The authors have no conflicts of interest to declare.
Please cite this article as: Adams, H., Kiesel, H., Andreae, B., Burdick, K., Elwood, C., Henson, J., Livingston, L., & Mix, N. (2026). Collaborative care in action: Early reflections from a simulation event on complex pain management. Simulation Technology & Operations Resource Magazine, 5(1), page-page. ISSN: 3070-3506.
ABSTRACT
Chronic pain remains a public health concern, often requiring coordinated, interdisciplinary care for effective management. Despite the prevalence of pain, prelicensure healthcare education has a limited focus on preparing learners to manage pain via interprofessional collaboration. This manuscript describes the design, implementation, and early reflections from a simulation-based interprofessional education (IPE) event focused on interdisciplinary pain care. The event involved 95 students from five health professions who worked in interdisciplinary teams (IDT) to manage a simulated patient experiencing chronic pain following a work-related injury and surgical intervention.
Grounded in constructivist and social learning theories, the simulation employed an interdisciplinary pain clinic model, incorporating structured prebriefing, profession-specific assessment simulations, a collaborative care conference, and a student-led debrief. Learning objectives for the event emphasized interprofessional competencies related to communication, understanding roles, and patient-centered care. Learner active participation and peer observation were used as instructional methods to maximize learning while addressing common resource constraints.
Students reported that the event enhanced their understanding of collaborative care and the specific roles of different professions in pain management. Feedback emphasized the effectiveness of the realistic environment, including the use of SP methodology, in preparing them for the complexities of managing chronic pain. The high-fidelity, interdisciplinary pain clinic model facilitated meaningful participation in collaborative pain management. Its scalable and practical design demonstrates the potential for broader adoption in healthcare education to foster interprofessional collaboration and prepare learners for best practice clinical pain care.
SECTION TITLE
STORM highlights exemplar work contributing to the advancement of healthcare simulation operations. All submissions are peer reviewed before publication in the STORM special edition of the SSH Simulation Spotlight. With articles covering training, policy & procedure, emerging technologies, and professional development, STORM has everything needed to stay current and well-rounded in the pursuit of simulation operations excellence.
STORM highlights exemplar work contributing to the advancement of healthcare simulation operations. All submissions are peer reviewed before publication in the STORM special edition of the SSH Simulation Spotlight. With articles covering training, policy & procedure, emerging technologies, and professional development, STORM has everything needed to stay current and well-rounded in the pursuit of simulation operations excellence.
INTRODUCTION
Chronic pain is a costly public health burden in the United States and globally (Rice et al., 2015). As many as 24.3% of U.S. adults report experiencing chronic pain in the past 3 months, making pain the most common reason for seeking medical care (Lucas & Sohi, 2024; St Sauver et al., 2012; United States Department of Health and Human Services, 2025). The complex, multidimensional nature of chronic pain often leads to unmet needs among those most affected (Cohen et al., 2021), including treatment for mental health disorders, opioid medication management, and support with social integration (Baker et al., 2024; Bannon et al., 2021; De La Rosa et al., 2024). The current U.S. healthcare system can lead to fragmented care, placing individuals with chronic pain at increased risk of mismanagement. This risk is especially pronounced in rural and non-metropolitan areas, where access to healthcare professionals is limited, despite a higher prevalence of disabling chronic pain (Lucas & Sohi, 2024; Thomas et al., 2024).
Despite frequently encountering patients in pain, healthcare providers remain underprepared to manage it, according to a 2011 U.S. Institute of Medicine report (Institute of Medicine, 2011). Effective care for individuals with chronic pain requires a range of knowledge and skills, including a collaborative, interprofessional approach to assessment and treatment planning. However, prelicensure healthcare education often lacks instruction on the value of interdisciplinary teamwork, as training programs remain siloed, particularly in professional schools (Hodgson et al., 2019). Improving the pain education delivered to prelicensure healthcare students is one recommended strategy to address pain as a public health priority by augmenting provider preparedness (National Institutes of Health & Institute of Medicine, 2022).
Although recommended interprofessional pain education curricula and core competencies exist, their integration into prelicensure training remains limited. Simulation-based education offers a promising strategy to bridge this gap and enhance interprofessional learning in pain management (Fishman et al., 2013; Gordon et al., 2018; International Association for the Study of Pain, 2018). It provides a safe, immersive environment for learners from diverse healthcare backgrounds to engage in realistic, team-based clinical scenarios (Al-Elq, 2010; Armstrong et al., 2024; Durham & Alden, 2008). Research supports the use of interprofessional curricula to improve students’ attitudes and understanding of collaborative roles (Saragih et al., 2024; Spaulding et al., 2019).
However, scaling simulation for large interprofessional cohorts presents challenges, particularly due to the significant resources required. As a result, pain-focused interprofessional education (IPE) events often rely on paper-based case discussions rather than high-fidelity simulations due to resource limitations (Garwood et al., 2022; Institute of Medicine, 2015; Langford et al., 2019; Watt-Watson et al., 2018). Overcoming these barriers is essential to fully leverage simulation’s potential in preparing future healthcare professionals to manage the complexities of chronic pain.
In response to the challenges of implementation of interprofessional simulations, the following interdisciplinary simulation event was designed and rooted in social and constructivist learning theories. This manuscript outlines the structure of the IPE event, which used a complex chronic pain case to provide a realistic context for practicing interprofessional collaboration within an interdisciplinary pain clinic setting.
While the formal learning objectives for this event centered on developing interprofessional collaborative practice competencies, the chronic pain case was deliberately chosen as the vehicle for this experience. Chronic pain inherently requires integrated, team-based care, making it an ideal context for students to observe and discuss how different healthcare professions approach assessment, treatment, and patient management. Although providing optimal pain management itself was not a direct objective, the scenario organically promoted learning in this area by exposing students to the diverse perspectives and decision-making process involved in chronic pain care.
EVENT PLANING AND DESIGN
Planning for the simulation event began roughly 10 months before the scheduled event date, with faculty and simulation center staff meeting monthly to organize and develop the event. The simulation event was designed to manage a simulated patient (SP) with chronic pain using an interdisciplinary pain clinic model. Simulation staff and faculty from occupational therapy (OT), physical therapy (PT), athletic training (AT), physician assistant studies (PA), and social work (SW) collaboratively developed the case. The case involved a patient experiencing chronic pain following a worksite injury and subsequent surgical procedure. Physical limitations, disruptions to daily activities, household tasks, and work, symptoms of mood disorder, and a history of substance abuse were incorporated into the patient case. The simulated patient was a firefighter, necessitating high functional capabilities to return to unrestricted duty. The complexity of the case encouraged students to collaborate and determine each team member’s contribution to the holistic care plan.
The event was designed with the following learning objectives in mind, ensuring a comprehensive approach to interprofessional education in pain management. The event's learning objectives focused on interprofessional collaborative practice, and the chronic pain scenario served as the context for applying these competencies in a realistic, team-based case.
Work with individuals of other professions to maintain a climate of mutual respect and shared values.
Use the knowledge of one’s own role and those of other professions to appropriately assess and address the health needs of patients and to promote and advance the health of populations.
Communicate with patients, families, communities, and professionals in health and other fields in a responsive and responsible manner that supports a team approach to the promotion and maintenance of health and the prevention and treatment of disease.
Apply relationship-building values and the principles of team dynamics to perform effectively in different team roles to plan, deliver, and evaluate patient/population-centered care and population health programs and policies that are safe, timely, efficient, effective, and equitable.
FORMATION OF INTERDISCIPLINARY TEAMS
A total of 95 students from five health professions participated in this interprofessional collaborative care simulated learning event. The participants included 20 OT, 32 PT, 6 AT, 28 PA, and 9 SW students. All students had prior simulation and clinical experiences.
Prior to the event, students were divided into six interdisciplinary teams (IDT), ensuring representation from all professions in each group. Each group had approximately 15 students. Three IDTs were scheduled to engage in the interprofessional learning event each day. Each student was required to participate in the event for eight hours in a single day. This approach allowed the team to leverage available resources effectively, although it necessitated two days of facilitation.
RESOURCE AND PERSONNEL NEEDS
The simulation event was held at a local healthcare education center, which included a simulated clinic space and several classrooms. Each exam room was equipped with cameras and microphones for remote viewing, allowing students to observe in real-time from a classroom.
A total of six individuals facilitated the event each day, including three faculty members and three simulation staff. One faculty member and one simulation staff member were assigned to each of the three IDT rooms. Additionally, three simulated patients (SPs) participated daily, with one SP assigned to each IDT. Each SP discussed their needs and challenges as outlined in the case notes with their assigned IDT. With additional resources, expanding the number of facilitators could introduce more diverse perspectives and further enrich the student learning experience.
SIMULATION EVENT TIMELINE
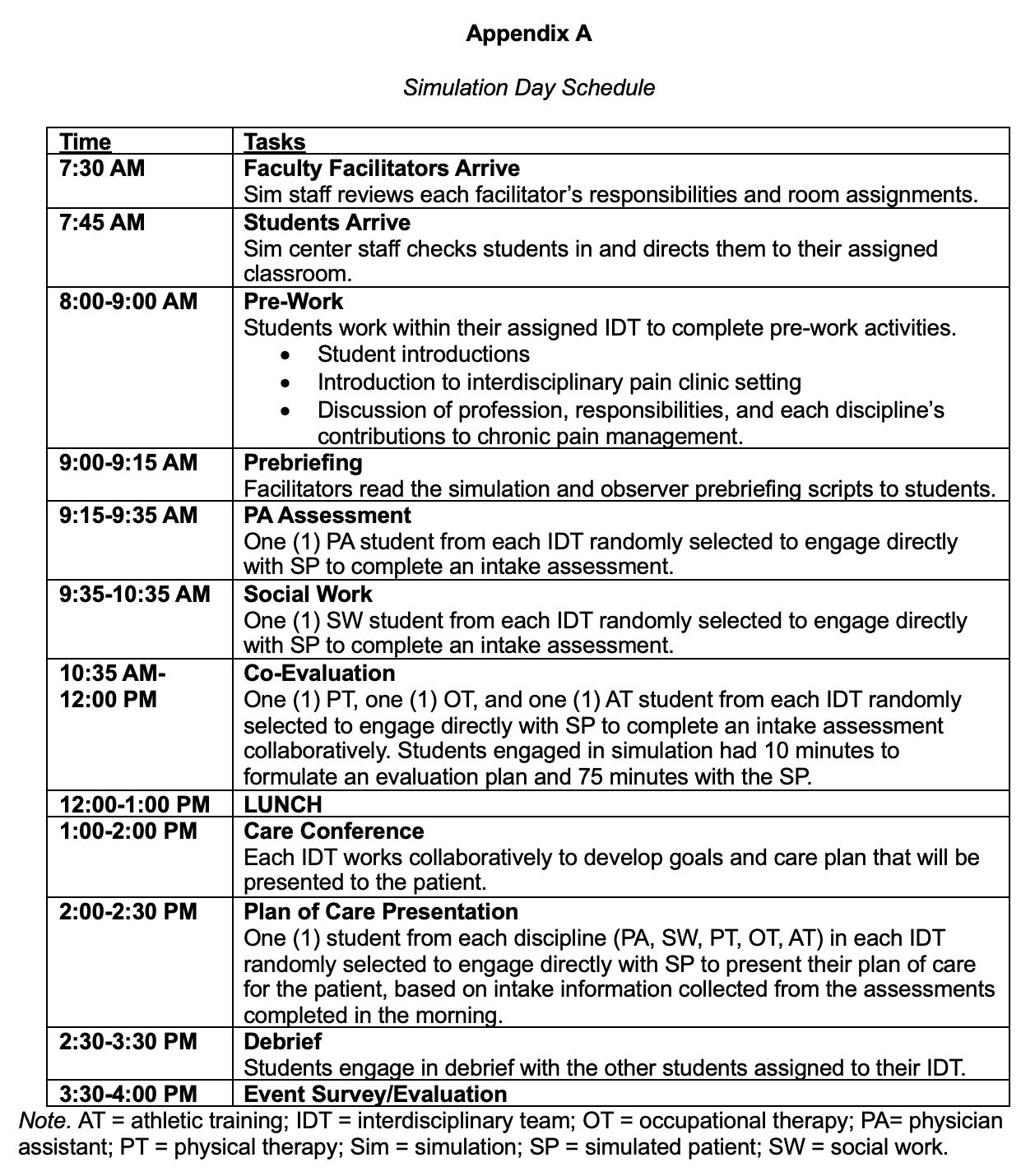
An overview of the day’s timeline is provided in Appendix A. All faculty facilitators were provided with this timeline to ensure consistency across rooms. Below you will find more detailed descriptions of each session.
Student Arrival and Prebriefing
Upon arrival, students were divided into classrooms based on IDT group assignments. They completed a 60-minute prebrief session, which included introductions and a group discussion about each discipline’s roles and responsibilities, with a focus on each profession’s perspective on pain management. Facilitators provided objectives and instructions at the beginning of the prebrief session, but students were tasked with leading the discussion based on their assigned tasks.
Morning Simulation Sessions
Following the prebrief group discussion, facilitators briefed all students on the simulation schedule and objectives for the assessment simulations. The facilitators then randomly selected one student from each discipline to participate in the assigned assessment simulations, informing selected students just before the start of each simulation (see the schedule below). Time limitations for all assessment simulations were determined based on faculty guidance and established best practices. Non-selected students observed remotely from the classroom with the rest of their IDT. Students were encouraged to engage in a collaborative discussion with their IDT and utilize the information obtained from each assessment to strategize subsequent encounters with the SP. The IDT also collaborated for ten minutes prior to the AT, PT, and OT simulation to develop a logical plan for their co-evaluation. Below is the simulation schedule:
PA Assessment (1 PA student) – 20 minutes
SW Assessment (1 SW student) – 60 minutes
AT, PT, OT Co-Assessment (1 AT, 1 PT, 1 OT student) – 75 minutes
Afternoon Collaborative Care Conference
After lunch, students met in their IDT for a 60-minute collaborative care conference. Facilitators provided objectives for the conference around establishing goals related to pain management, improved function, quality of life, and creating a well-defined plan of care that incorporated all disciplines. Students independently facilitated their group discussion after receiving verbal objectives. The video conferencing platform Zoom was utilized in each classroom, allowing facilitators to observe the IDT’s discussion from a separate room.
Care Plan Presentation, Debrief, and Assessment
At the end of the care conference, one student from each discipline was randomly selected to present their IDT’s plan of care to the SP, with preference given to those who had not participated in the assessment simulations. This simulation took place in a conference room and was recorded, allowing non-participating students to observe from the classroom. Faculty watched remotely, in a separate space from the students.
The day concluded with a 60-minute group debrief amongst each IDT. The session was guided by an adapted version of an interprofessional debriefing guide developed by the University of Kansas Medical Center (University of Kansas Medical Center, n.d.). To promote open dialogue and interprofessional engagement, students were instructed to sit in a circle and avoid sitting next to peers from their own discipline. After receiving session objectives, discussion instructions, and a debriefing question guide, students were encouraged to facilitate the conversation independently, with faculty and staff available for support if needed. This session emphasized the importance of interprofessional collaborative practice, including teamwork, effective communication, and understanding the roles and responsibilities of different healthcare professionals. Additionally, the debrief discussion covered approaches to managing chronic pain, with a focus on mental health, quality of life, and substance use concerns.
Following the debrief session, both quantitative and qualitative data were collected through a post-event survey that assessed learning outcomes and student perceptions of the simulation event. Qualitative comments and feedback were positive, noting improved clarity of professional roles, stronger appreciation for team-based decision-making, and improved confidence in communicating within an interdisciplinary pain-management context. Data collection is planned to continue with a subsequent cohort, and quantitative analysis will be conducted after all data is gathered, with results to be reported in future manuscripts.
DISCUSSION OF EDUCATIONAL ADVANTAGE
The simulation-based learning event was designed to provide healthcare students with a realistic opportunity to collaboratively evaluate and plan treatment for a patient experiencing chronic pain. To support this goal, the simulation design incorporated simulated patients as the selected modality, enhancing authenticity and reinforcing learning objectives focused on compassionate care and empathy. The event structure included a prebrief, the simulation activity, and student-led debriefings, providing a comprehensive learning experience. The event was grounded in a simulated interdisciplinary pain clinic, a best-practice clinical model to treat complex pain (Gatchel et al., 2014). This model aligns with current standards in clinical care and provides an ideal context for fostering interprofessional communication and collaboration, skills that are often underdeveloped in traditional healthcare education (Hodgson et al., 2019). Given that many students have limited exposure to this model during their clinical training, the event served as a valuable supplement to their educational experience.
General feedback from students supported the use of the interdisciplinary pain clinic model for the simulation event. Students found the patient case and setting realistic and appreciated the safe environment that encouraged peer engagement. Students viewed the experience as distinct from other IPE simulations or clinical opportunities, highlighting the relevance of this event to real-world practice.
The educational event design was informed by constructivist learning theory and Bandura’s social learning theory, emphasizing learning through experience, observation, and reflection (Bandura, 1976; Dieckmann, 2009; Taylor & Hamdy, 2013). To address common challenges in interprofessional simulation, particularly scalability and resource limitations, not all students participated directly in the simulation. Instead, some students observed their peers, enabling them to model effective behaviors and critically reflect on team dynamics, communication strategies, and clinical decision-making. The simulation structure preserved the educational value of the experience while enabling broader participation without requiring extra resources.
During the debrief, faculty identified a consistent theme- students valued the opportunity to witness how other professionals approach patient care, especially during initial assessments. The interprofessional event enhanced students’ understanding of the capabilities and limitations of various disciplines and fostered greater respect for the roles each profession plays in collaborative care. Student reflections on their assigned roles, either as active participants or observers, varied. Some students expressed a preference for direct engagement with the SP, while others valued the observer role, appreciating its lower-pressure environment, which allowed them to focus more deeply on team dynamics, interprofessional communication, and clinical reasoning without the added demands of a performance-based role.
The interprofessional simulation event provided significant educational value in bringing together students from five healthcare disciplines to manage an individual with chronic pain. Students engaged in collaborative learning, fostering their understanding of each profession's contributions to care while developing teamwork, communication, empathy, and patient-centered care skills. This event has several limitations, including being conducted at a single site with students from only one university. In addition, the event lacked representation from psychologists, a common inclusion in interdisciplinary pain clinics (Brecht et al., 2020). Despite these limitations, the event highlighted the value and importance of interdisciplinary approaches to managing chronic pain. The absence of certain disciplines, including psychology and nutrition/wellness, emerged as a key discussion point during the debrief, particularly when considering additional professional perspectives that could enhance patient care.
The simulation provided a high-fidelity learning environment, allowing students an opportunity to experience the nuances and challenges of collaborative pain management in a controlled setting. The simulation-based event design is scalable and practical, relying primarily on standard simulation equipment and faculty coordination. It effectively delivers educational outcomes that are difficult to achieve through traditional didactic methods. The simulation-based event demonstrates potential for adaptation across various healthcare education programs to support collaborative management of patients with multifaceted pain. The success of this interprofessional education event in fostering authentic collaboration and enthusiasm supports its continued implementation and expansion as an effective instructional strategy to prepare future healthcare providers for the collaborative realities of best practice clinical pain management.
REFERENCES
Al-Elq, A. (2010). Simulation-based medical teaching and learning. Journal of Family and Community Medicine, 17(1), 35. https://doi.org/10.4103/1319-1683.68787
Armstrong, K. J., Walker, S. E., Woofter, B. L., & Brown, A. N. (2024). Current uses of simulation and standardized patients in athletic training education: uses for teaching and assessment and barriers to use. Athletic Training Education Journal, 19(3), 173–184. https://doi.org/10.4085/1947-380x-23-041
Baker, M. B., Liu, E. C., Bully, M. A., Hsieh, A., Nozari, A., Tuler, M., & Binda, D. D. (2024). Overcoming Barriers: A comprehensive review of chronic pain management and accessibility challenges in rural America. Healthcare, 12(17), 1765. https://doi.org/10.3390/healthcare12171765
Bandura, A. (1976). Social learning theory. Englewood Cliffs, NJ: Prentice-Hall.
Bannon, S., Greenberg, J., Mace, R. A., Locascio, J. J., & Vranceanu, A. (2021). The role of social isolation in physical and emotional outcomes among patients with chronic pain. General Hospital Psychiatry, 69, 50–54. https://doi.org/10.1016/j.genhosppsych.2021.01.009
Brecht, D. M., Stephens, J., & Gatchel, R. J. (2020). Interdisciplinary Pain Management Programs in the Treatment of Pain Conditions. In Pain Management for Clinicians (pp. 461–489). https://doi.org/10.1007/978-3-030-39982-5_18
Cohen, S. P., Vase, L., & Hooten, W. M. (2021). Chronic pain: an update on burden, best practices, and new advances. The Lancet, 397(10289), 2082–2097. https://doi.org/10.1016/s0140-6736(21)00393-7
De La Rosa, J. S., Brady, B. R., Herder, K. E., Wallace, J. S., Ibrahim, M. M., Allen, A. M., Meyerson, B. E., Suhr, K. A., & Vanderah, T. W. (2024). The unmet mental health needs of U.S. adults living with chronic pain. Pain, 165(12), 2877–2887. https://doi.org/10.1097/j.pain.0000000000003340
Dieckmann, P. (Ed.) (2009). Using simulations for education, training, and research. Pabst Science Publishers.
Durham, C. F., & Alden, K. R. (2008, April 1). Enhancing patient safety in nursing education through patient simulation. Patient Safety and Quality. http://www.ncbi.nlm.nih.gov/books/NBK2628/
Fishman, S. M., Young, H. M., Arwood, E. L., Chou, R., Herr, K., Murinson, B. B., Watt-Watson, J., Carr, D. B., Gordon, D. B., Stevens, B. J., Bakerjian, D., Ballantyne, J. C., Courtenay, M., Djukic, M., Koebner, I. J., Mongoven, J. M., Paice, J. A., Prasad, R., Singh, N., . . . Strassels, S. A. (2013). Core Competencies for Pain Management: Results of an Interprofessional Consensus Summit. Pain Medicine, 14(7), 971–981. https://doi.org/10.1111/pme.12107
Garwood, C., Banfill, K., Maher, S., McQueen, J., R Moser, L., Moul, A., & Walczyk, M. (2022). A multimodal interprofessional education program including case-based problem solving focused on pain management increases student’s knowledge and interprofessional skills. Journal of Interprofessional Care, 36(6), 864–872. https://doi.org/10.1080/13561820.2022.2038102
Gatchel, R. J., McGeary, D. D., McGeary, C. A., & Lippe, B. (2014). Interdisciplinary chronic pain management: Past, present, and future. American Psychologist, 69(2), 119–130. https://doi.org/10.1037/a0035514
Gordon, D. B., Watt-Watson, J., & Hogans, B. B. (2018). Interprofessional pain education—with, from, and about competent, collaborative practice teams to transform pain care. PAIN Reports, 3(3), e663. https://doi.org/10.1097/pr9.0000000000000663
Hodgson, J., Moore, K., Acri, T., & Treisman, G. J. (2019). Integrative medicine for vulnerable populations. https://doi.org/10.1007/978-3-030-21611-5
Institute of Medicine. (2011). Relieving pain in America. In National Academies Press eBooks. https://doi.org/10.17226/13172
Institute of Medicine. (2015). Measuring the impact of interprofessional education on collaborative practice and patient outcomes. In National Academies Press eBooks. https://doi.org/10.17226/21726
International Association for the Study of Pain. (2018). IASP Curricula. https://www.ninds.nih.gov/sites/default/files/documents/NationalPainStrategy_508C.pdf
Langford, D. J., Gordon, D. B., Loeseer, J. D., Tauben, D. J., & Doorenbos, A. Z. (2019). Evaluation of an interprofessional active learning session on acute pain and opioid use disorder using the interprofessional collaborative competency attainment scale. Journal of Interprofessional Care, 34(2), 193–201. https://doi.org/10.1080/13561820.2019.1629398
Lucas, J. W., & Sohi, I. (2024). Chronic pain and high-impact chronic pain among U.S. Adults, 2023 (Issue 518). https://doi.org/10.15620/cdc/169630
National Institutes of Health & Institute of Medicine. (2022, July 11). National pain strategy: A comprehensive population health strategy for pain. National Institute of Neurological Disorders and Stroke. https://www.ninds.nih.gov/sites/default/files/documents/NationalPainStrategy_508C.pdf
Rice, A. S., Smith, B. H., & Blyth, F. M. (2015). Pain and the global burden of disease. Pain, 157(4), 791–796. https://doi.org/10.1097/j.pain.0000000000000454
Saragih, I. D., Hsiao, C., Fann, W., Hsu, C., Saragih, I. S., & Lee, B. (2024). Impacts of interprofessional education on collaborative practice of healthcare professionals: A systematic review and meta-analysis. Nurse Education Today, 136, 106136. https://doi.org/10.1016/j.nedt.2024.106136
Spaulding, E. M., Marvel, F. A., Jacob, E., Rahman, A., Hansen, B. R., Hanyok, L. A., Martin, S. S., & Han, H. (2019). Interprofessional education and collaboration among healthcare students and professionals: a systematic review and call for action. Journal of Interprofessional Care, 35(4), 612–621. https://doi.org/10.1080/13561820.2019.1697214
St Sauver, J. L., Warner, D. O., Yawn, B. P., Jacobson, D. J., McGree, M. E., Pankratz, J. J., Melton, L. J., Roger, V. L., Ebbert, J. O., & Rocca, W. A. (2012). Why patients visit their doctors: Assessing the most prevalent conditions in a defined American population. Mayo Clinic Proceedings, 88(1), 56–67. https://doi.org/10.1016/j.mayocp.2012.08.020
Taylor, D. C. M., & Hamdy, H. (2013). Adult learning theories: Implications for learning and teaching in medical education: AMEE Guide No. 83. Medical Teacher, 35(11), e1561-e1572. https://doi.org/10.3109/0142159X.2013.828153
Thomas, K. H., Dalili, M. N., Cheng, H., Dawson, S., Donnelly, N., Higgins, J. P. T., & Hickman, M. (2024). Prevalence of problematic pharmaceutical opioid use in patients with chronic non‐cancer pain: A systematic review and meta‐analysis. Addiction, 119(11), 1904–1922. https://doi.org/10.1111/add.16616
United States Department of Health and Human Services. (2025, February 23). Pain. National Center for Complementary and Integrative Health. Retrieved May 30, 2025, from https://www.nccih.nih.gov/health/pain
University of Kansas Medical Center. (n.d.). General Interprofessional Debriefing Questions Facilitator guide. https://www.kumc.edu/documents/ciper/General%20Interprofessional%20Debriefing%20Questions%20Facilitator%20Guide.pdf
Watt-Watson, J., McGillion, M., Lax, L., Oskarsson, J., Hunter, J., MacLennan, C., Knickle, K., & Victor, J. C. (2018). Evaluating an Innovative eLearning Pain Education Interprofessional Resource: a Pre–Post Study. Pain Medicine, 20(1), 37–49. https://doi.org/10.1093/pm/pny105
Appendix A